
It is also the health professional's responsibility to verify the applicable rules and regulations relating to drugs and medical devices at the time of prescription. 
Nor do the ESC Guidelines exempt health professionals from taking into full and careful consideration the relevant official updated recommendations or guidelines issued by the competent public health authorities, in order to manage each patient's case in light of the scientifically accepted data pursuant to their respective ethical and professional obligations. Health professionals are encouraged to take the ESC Guidelines fully into account when exercising their clinical judgment, as well as in the determination and the implementation of preventive, diagnostic or therapeutic medical strategies however, the ESC Guidelines do not override, in any way whatsoever, the individual responsibility of health professionals to make appropriate and accurate decisions in consideration of each patient's health condition and in consultation with that patient and, where appropriate and/or necessary, the patient's caregiver. The ESC is not responsible in the event of any contradiction, discrepancy and/or ambiguity between the ESC Guidelines and any other official recommendations or guidelines issued by the relevant public health authorities, in particular in relation to good use of healthcare or therapeutic strategies. 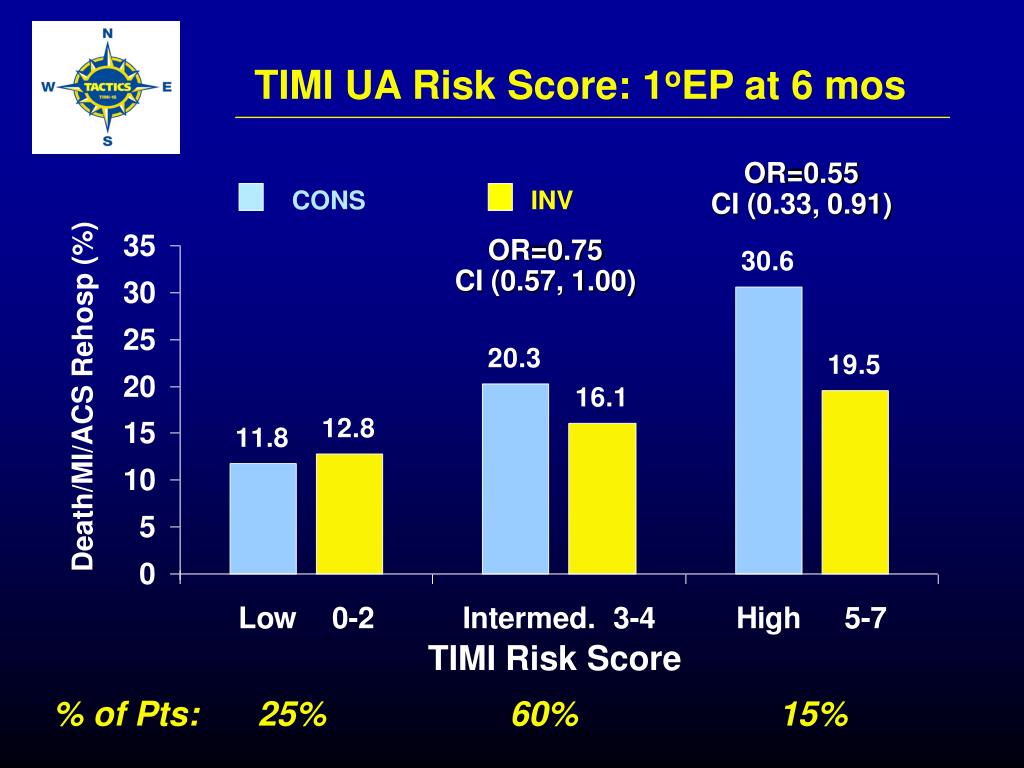
Disclaimer: The ESC Guidelines represent the views of the ESC and were produced after careful consideration of the scientific and medical knowledge and the evidence available at the time of their publication. (TIMI score 03) and 50.6 into the high-risk score The intended treatment, either conservative ther- group (TIMI score 47). Killips categorization grade 2-4 had the highest relative risk (RR-15.85) of the seven potentially dubious variables evaluated, followed by systolic BP 100mmHg (RR-10.48), diabetes mellitus (RR-2.79), and age >65 years (RR- 2.59).Ĭonclusions: In patients with STEMI, the TIMI risk scoring system appears to be a straightforward, valid, and practical bedside tool for quantitative risk classification and short-term prognosis prediction.Permission can be obtained upon submission of a written request to Oxford University Press, the publisher of the European Heart Journal and the party authorized to handle such permissions on behalf of the ESC. The highest mortality rate (total 17 deaths) was found in the high-risk group (55.6%), followed by moderate-risk (12.2%) and low-risk (1.28%) groups, respectively. The GRACE risk score requires 8 variables to assess risk of in-hospital mortality, as follows: age, heart rate, systolic blood pressure, Killip classification. Results: According to the TIMI risk score, 79 patients (54.5%) had low-risk, 48 (33.1%) to the moderate-risk, and 18 (12.4%) to the high-risk. strategy is the TIMI risk score, which is based upon seven variables available at presentation. All patients received standard anti-ischemic medication, were thrombolyzed, monitored in the ICCU, and monitored throughout their hospital stay for post-MI sequelae. Based on their TIMI scores, the patients were placed into three risk groups: low-risk,moderate-risk, and high-risk. 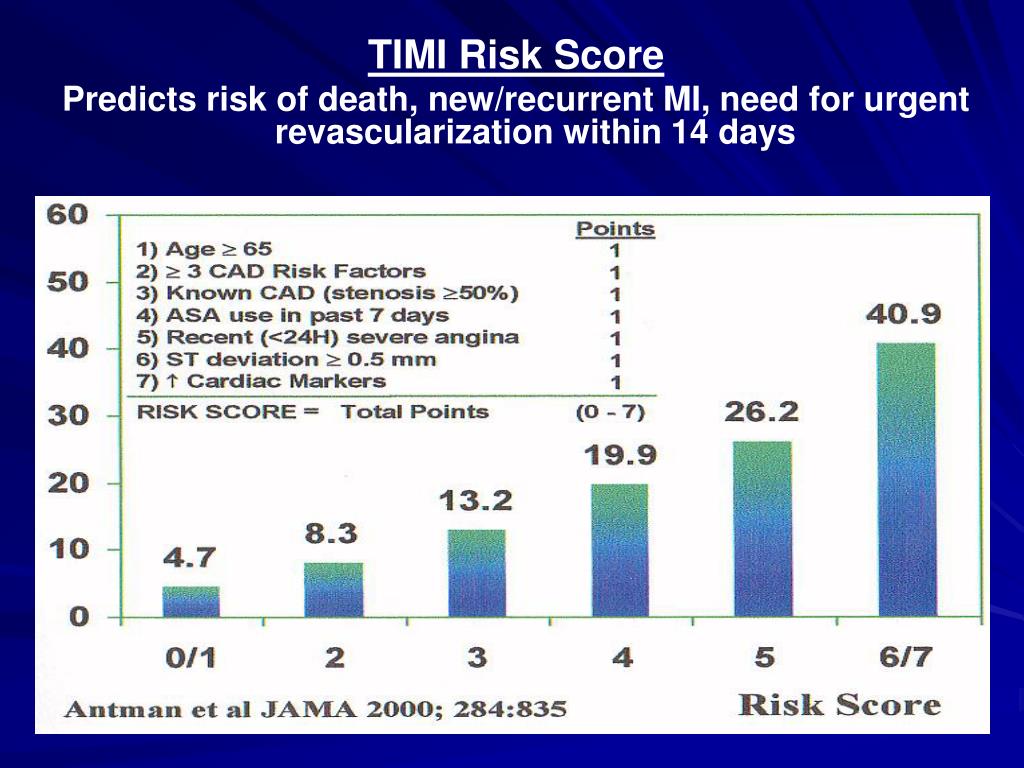
Methods: 145 STEMI patients were included in this srudy, TIMI risk scores were calculated and analysed vis-Ã -vis various relevant parameters. An attempt was made to assess the situation by comparing risk stratification based on the TIMI score with the hospital outcome of such individuals. Background: The Thrombolysis in Myocardial Infarction (TIMI) risk score is said to be an important factor in predicting mortality risk in fibrinolysis-eligible STEMI patients.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
